Those who develop pancreatitis will need to make dietary changes as the most critical part of their treatment plan. Severe cases may also require medical management.
Treatment Options
Diet
Fasting is recommended until the inflammation subsides, and often, that requires hospitalization to monitor. Once controlled, diet shifts to clear liquids and bland foods. For persistent inflammation, it might be necessary to consider a feeding tube to ensure proper nutrition.
Medications
Pain management is critical for this condition. Any medications will focus on controlling pain to allow for proper healing.
Pancreatic enzyme supplements taken with each meal can help the body break down nutrients, allowing the pancreas time to heal.
IV Fluids
Intravenous fluids can prevent dehydration as the pancreas heals.
Alcohol Abuse Treatment
For individuals who consume alcohol in large quantities, it might be necessary to seek treatment to stop. Daily alcohol consumption is one of the primary causes of pancreatitis, and continuing to drink can lead to serious complications.
Surgery
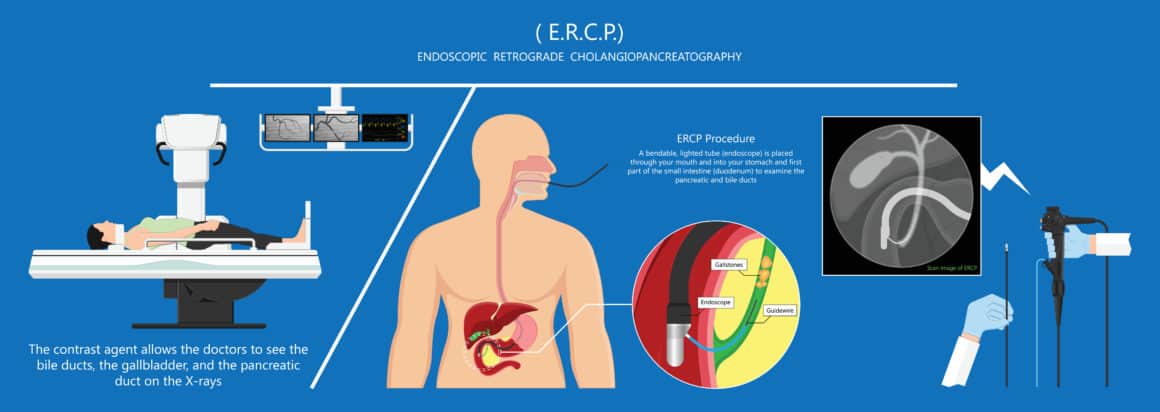
There are several potential surgical procedures that a physician may consider to prevent further bouts of pancreatitis. Endoscopic retrograde cholangiopancreatography (ERCP) is a minimally invasive procedure that allows the medical team to look at the patient’s pancreas and bile ducts and make repairs if necessary.
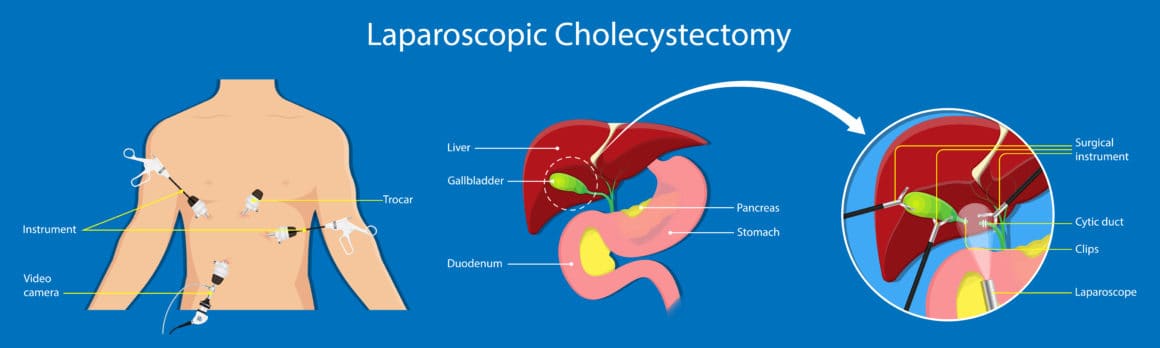
Cholecystectomy is the removal of the gallbladder. It may be part of the treatment for those with gallstones. In some cases, the surgeon may need to drain fluid from the pancreas and remove dead or damaged tissue from the organ.
Lifestyle Changes
Lifestyle changes, including quitting smoking and eliminating alcohol from the diet, are critical parts of the treatment for pancreatitis. In addition, your healthcare provider might recommend switching to a low-fat diet with an emphasis on fruit and vegetables plus lean protein.
It’s essential to drink plenty of fluid when healing from pancreatitis, as well. The condition can lead to dehydration, so increased fluid intake and possibly IV fluids are necessary to counteract that side effect.
Alternative Medicine
Alternative therapies alone will not promote healing of the pancreas, but they can work in conjunction with traditional treatments, especially when it comes to pain management. The pain of pancreatitis, especially the chronic condition, may be difficult to control through drug therapies alone.
Alternative treatment options like medication, relaxation exercises, yoga, and acupuncture might help control pain, which, in turn, will promote natural healing. Patients should always consult with their healthcare provider before adding any new form of alternative treatment to their pancreatitis management plan.
FAQ
How long does pancreatitis take to heal?
It will depend on the severity of the inflammation and how well it heals. For some, the condition may clear up in a week; for others, it will take several weeks of restricted eating. Those who have surgery may take longer to heal.
What brings on a pancreatitis attack?
For some, it will be excessive alcohol consumption; for others, it may be diet choices or an underlying condition, such as gallstones. Heavy drinking causes up to 70 percent of chronic pancreatitis cases; so, avoiding alcohol is important. Smoking may also be a contributing factor as it can lead to a progression of the disease and, possibly, pancreatic cancer.
Is pancreatitis life-threatening?
It can be in severe cases. Inflammation can lead to infection, and that can be life-threatening.
Persistent pancreatitis can come with other complications, as well, such as pancreatic cancer. Other possibilities include:
- a pseudocyst that can rupture and cause internal bleeding,
- kidney failure,
- low oxygenation of the blood (hypoxemia),
- diabetes, and
- malnutrition.
Each of these conditions is very serious and can lead to death.
Disclaimer: this article does not constitute or replace medical advice. If you have an emergency or a serious medical question, please contact a medical professional or call 911 immediately. To see our full medical disclaimer, visit our Terms of Use page.




